What Do Value Assessments Miss? Rethinking Value Using New Health Economics Evidence.
November 11, 2019
An Interview with Dr. Anupam B. Jena, MD, PhD, Scientific Advisor, Precision Xtract.

Patti Peeples, R.Ph., PhD, is founder and CEO of HealthEconomics.com and Principal Researcher for the HE Institute. At the forefront in health economics and market access for over 25 years, Dr. Peeples has extensive experience in the global pharmaceutical industry, pharmacy practice, medical communications, and entrepreneurship.
Anupam B, Jena, MD, PhD, Scientific Advisor for Precision Xtract, is a noted physician and economist whose research focuses on the economics of medical innovation, the economics of medical practice, healthcare productivity, and medical malpractice. He has published extensively in leading medical, economics, and health policy journals, and his work has been cited in The Wall Street Journal and The New York Times.
Dr. Peeples recently sat down with Dr. Jena to discuss his latest research with Precision Xtract that expands the definition and measurement of value of novel therapies by using new health economics evidence.
Dr. Peeples: What factors are driving the need to rethink today’s healthcare value conversation vs the kind of conversations we had 5 to 10 years ago?
Dr. Jena: As drug prices continue to climb and our society wrestles with paying for novel therapies, my colleagues and I have explored how value assessment approaches need to be reconsidered. When thinking about the value of new treatments and technologies, I believe we need to start at the top of the pyramid, so to speak. Healthcare competes for other societal resources, such as education, defense, or infrastructure. To make informed decisions about resource allocation and return on investment, then we – as an industry – need to have a conversation about how we more comprehensively value these interventions.
One of the areas of opportunity that arises when performing value assessments is the identification of where our dollars are being spent on low-value care. By redirecting spending on low-value care towards high-value care, we can raise population health at the same total cost. Moreover, many high value services are the product of innovation, and this re-allocation toward high-value care can increase the return and likelihood of downstream innovation.
There are several other factors that have transformed our value assessment approaches. Over the past decade, we have seen drug therapy move away from chronic disease management in favor of new innovations that offer the promise of curing or significantly modifying diseases such as cancer, HIV, and hepatitis C (HCV), among others. We also have come to recognize that patient-reported outcomes and real-world evidence (RWE) are very important in evaluating new drugs and need to be incorporated into value assessments. Additionally, new healthcare delivery and financial models are transforming the way medical care is delivered, and reimbursement is moving to a value-based model that rewards patient and economic outcomes. New innovations are increasingly expensive, and their value needs to be measured in a broader context to avoid the imposition of arbitrary barriers to patient access that result from focusing exclusively on cost. And lastly, we are increasingly having a public policy debate that asks, “who should be valuing these new interventions?”. The answer to this question is pivotal to value assessment. In a recent white paper, I present a framework for a more comprehensive value assessment.

What do patients value? What does society value? How should we be aligning the prices of new drugs, devices, and other technologies with those values, especially if those values differ?
Anupam B. Jena, MD, PhD
Dr. Peeples: What dimensions should we be considering in a new approach to value, specifically for innovative healthcare technologies?
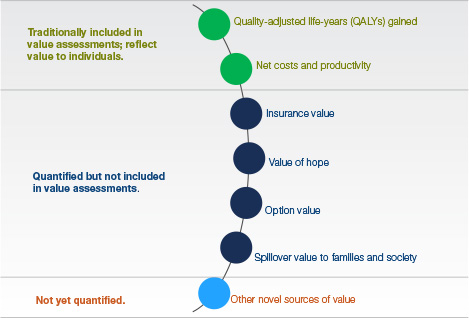
Dr. Jena: Traditionally, we’ve measured value in healthcare using quality-adjusted life years (QALYs), incorporating health benefits, cost, and productivity impact. However, this traditional assessment misses a number of new dimensions that may have a significant impact on overall value.
For instance, insurance value is the amount a consumer is willing to pay to protect themselves against financial and health losses for a rare, but expensive disease. Extending this concept to prescription drugs, it is the value a consumer places on the drug being available even if they never use it because the treatment is there for them some day if they, or a loved one, need it.
Another new dimension is the value of hope. Hope is the value that patients with a serious, life-threatening disease place on long-term treatment response. Using median survival rates as the outcome largely ignores the sub-group of patients who may receive a durable response to treatment. Some research suggests that patients value durable responses to treatment over incremental responses even when the likelihood of a durable response is much lower.
Additionally, option value is an important, but difficult to measure, dimension of value. In this type of value, a value option is placed by the patient on a new drug that offers meaningful therapeutic response but has limitations, such as serious adverse reactions, that limit its use to those patients who can tolerate it. For those patients who choose to utilize the drug, downstream improvements in therapy resulting from new innovations will be available that offer better outcomes. For these patients, the new drug offers possible access to an option they might otherwise not have had. A classic example of the value option may be seen with AZT, an agent with modest effectiveness and considerable side effects. A sub-set of patients were able to tolerate AZT, and thus lived long enough to receive safer, more effective antiviral therapy that resulted from the clinical and scientific knowledge that occurred over time.

Finally, there is the spillover effect. Drug utilization has an investment as well as a consumption component. For instance, drugs used for serious mental illnesses have the effect of reducing caregiver burden, crime, homelessness and other societal burdens. Vaccinations not only reduce the risk of a number of serious infections, but they also prevent the spread of diseases among the population at risk and reduce school and work absences.
Dr. Peeples: In an effort to shift the emphasis in healthcare from cost to value, you and your team have explored some innovative payment models. Can you describe some of these for pharmaceuticals and devices?
Dr. Jena: One of the areas of opportunity to shift thinking from cost to value is for sponsors to broaden their focus from comparing their product to the competitor product, and to think more broadly about how the intervention compares to all the other ways in which consumers spend their healthcare dollars. By expanding this view, it would facilitate us being able to identify low-value care alternatives in the healthcare delivery system that could be redirected toward higher value innovation.
We should really be thinking more broadly about how biopharmaceutical products or medical devices compare to all the other ways in which consumers spend their healthcare dollars.
Dr. Jena
Another opportunity is by employing innovative payment models, such as value-based contracting whereby reimbursement or payments to manufacturers are based on actual patient outcomes. In addition to value-based contracting, Precision Health Economics has also explored the use of subscription models or a pay-over-time amortization approach. These new models offer an opportunity to align price and value, while current pricing models based on short-term budgets and per member per month costs do not. Other new pricing models are being investigated including indication-based pricing, combination pricing, bundled payments, and tiered or capitated pricing.
Dr. Peeples: Where should we focus our efforts to drive the value conversation forward?
Dr. Jena: I think that the first step is to align stakeholders’ perspectives to a consensus on value assessment. This is one of the main objectives of our white paper (insert link here), which explains these concepts thoroughly. We will continue to improve assessment tools that use clinical and patient-reported outcomes as effectiveness outcomes and work on refining value measurements of insurance, option, spillover, and hope. Additionally, greater use of real-world evidence and the application of subgroup analyses to identify unique patient populations at higher risk of a disease need to be emphasized. Finally, the rapid introduction of specialty drugs and gene-based therapies need value estimation that captures the life-long benefits of these innovations to offset the concern about upfront expenditures (costs). By broadening our view and thinking comprehensively and rigorously about value, we can emphasize objectively the tradeoff between benefits to the patient and society and access to new innovations.
To download a complete copy of the white paper, What Do Value Assessments Miss? Rethinking Value Using New Health Economics Evidence, click the button below.






