Using AI, NLP and Data Visualization with RWE to Generate Insights into Care Gaps: Retrospective Cohort Analysis of Fracture Risk in Patients with Osteopenia and Osteoporosis
June 9, 2020
A sponsored blog by Veradigm®
SOURCE ARTICLE: Click here.

Real world data (RWD) are being used by an increasingly diverse group of stakeholders. As an example, patient advocacy groups are realizing the value they can offer to their communities by partnering with data analysis companies to explore treatment pathways, health outcomes, and patient-reported measures of disease and treatment impact. And as we know, the life sciences industry and payers are using real world evidence (RWE) to look at diagnostic approaches, unmet needs, and gaps in treatment.
This blog reports practical uses of RWD sourced from the largest, cloud-based electronic health record (EHR) platform in the United States, offered by Veradigm® as part of its Health Insights database. Preliminary data were first obtained using a cost-effective software-as-a-service application that enables transparent and efficient analysis of RWD. Information technology and data visualization tools were then used to evaluate unstructured data to identify care gaps and inform diagnosis and management of patients with osteoporosis or osteopenia who are at risk for bone fracture. The complete research approach is described in a White Paper.
Interested in this white paper? Email undine@scientist.com
RWE for Patient Advocacy Organizations
The National Osteoporosis Foundation (NOF) commissioned a study to examine the clinical and economic impact of new osteoporotic fractures suffered by Americans who were enrolled in the Medicare fee-for-service program. The NOF-sponsored study found that more than two million Medicare beneficiaries suffered 2.3 million fractures in CY 2015. Of these, 307,000 beneficiaries suffered one or more additional fractures for a total direct medical cost of $6.3 billion. It was estimated that about 50% of secondary fractures could have been avoided with appropriate osteopenia or osteoporosis treatment, and $1.2 billion could be saved by Medicare if 20% of repeat fractures were prevented. The study found that a small percentage—just 9%—of patients underwent bone mineral density (BMD) testing within six months of a new fracture.
Extracting Real World Data from Physician Notes in an EHR
Veradigm took the NOF study one step further and examined its ambulatory patient dataset for insights into patient cohorts and potential care gaps. The resulting retrospective cohort analysis explored BMD assessment in adult patients with or without a diagnosis of osteopenia or osteoporosis, based on ICD-9-CM and ICD-10-CM codes. Veradigm used Evalytica®, which offers powerful real-world evidence analytics, data visualization, and a cohort-building platform to enable real-time transparent analytics across diverse data sources, to collect preliminary data. The Evalytica analyses identified over 200,000 individuals with a diagnosis of osteopenia, osteoporosis, or other bone density or structure disorders who had at least one prescription for or documented use of osteoporosis medications.

Evalytica is software-as-a-service (SaaS) application that enables transparent and efficient analysis of EHR, registry, and administrative claims data that are available from diverse sources.
|
Natural Language Processing and Because DXA results were mainly entered by physicians into Subjective, Objective, Assessment, and Plan (SOAP) notes, natural language processing (NLP) techniques were used to identify, extract, and present the data in a structured format. DXA imaging results recorded by physicians consisted of the anatomy scanned (i.e., spine, forearms, or bones in the hip), the standardized score, and the score type.  |
As reported in the White Paper, the Evalytica analysis found that 81.9% of the total identified population were taking bisphosphonates, followed by a biologic (12.4%), SERMS (9.8%), and PTH or PTH analogs (2.9%). A subset of 10,064 patients had completed dual energy x-ray absorptiometry (DXA) scans, which compare a patient’s bone density with that of a 30-year-old healthy adult. Results are presented as T-scores, where the standard deviation (SD) between the patient’s bone density and that of the healthy control may be used to predict the likelihood of a future fracture. |
|
|
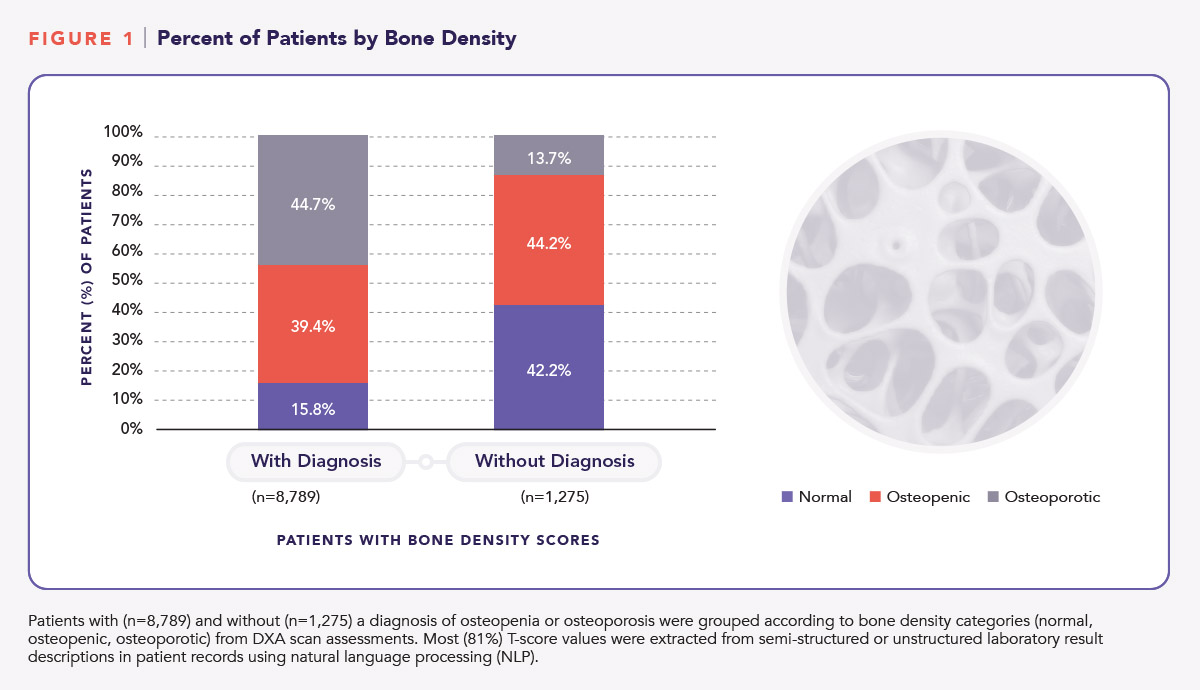
The power of artificial intelligence was used to derive essential information from physician notes within the EHR. For the analysis, 81% of T-scores were extracted from semi-structured and unstructured laboratory result descriptions using a machine learning-based NLP algorithm. T-scores derived from EHR using NLP were matched with diagnosis data. The percentages of patients with T-scores indicative of normal, osteopenic, or osteoporotic bone density are shown in Figure 1. For patients with a diagnosis, 39.4% had T scores indicative of osteopenia and 44.7% had T-scores corresponding to osteoporosis. For patients without a diagnosis, 44.2% and 13.7% had T-scores indicative of osteopenia and osteoporosis, respectively. |
||
Clinical Insights Derived from RWE Research
Even as providers work toward meeting therapeutic needs and improving outcomes, care gaps remain for a significant number of patients with osteopenia and osteoporosis. The analysis of de-identified patient data sourced from a Veradigm EHR revealed potential gaps in care for patients at risk of bone fracture.
- More than one-half of patients without a diagnosis for osteopenia or osteoporosis had recorded DXA scores suggestive of osteopenia or osteoporosis.
- Fully one-fifth of patients with a diagnosis and 6% of patients without a diagnosis had recorded T-scores of -3.0 or less (T-scores < -3.0 indicate “especially high risk” of future bone fractures).
Future Opportunities
As described in Veradigm’s White Paper, tools such as artificial intelligence, NLP, machine learning, and deep learning are digital capabilities with potential for supporting healthcare delivery and for providing timely clinical insights into high-risk populations by curating, qualifying, and exploring the full value of medical data. As demonstrated in the current analysis, when DXA scan results are recorded in narrative formats within unstructured fields in EHRs, natural language processing may enable consistent and efficient background T-score identification, extraction, and presentation.
Such data may also be used to examine medication adherence, persistence, and to identify areas of need for educational content to elevate health literacy with respect to bone health, modifiable risk factors, and the value of osteoporosis medications.
Veradigm is working towards full-scale adoption of artificial intelligence and related technologies for managing RWD available through its EHR platforms and registries.
|
Do you have a potential project that requires:
For more information on datasets and analytic services offered by Veradigm, contact us. |